COVID-19 has been the single greatest public health emergency in the history of the NHS.
The weeks ahead will be the hardest yet but I really do believe that we are entering the last phase of the struggle.
Because with every jab that goes into our arms, we are tilting the odds against Covid and in favour of the British people.
And, thanks to the miracle of science, not only is the end in sight and we know exactly how we will get there.
Boris Johnson
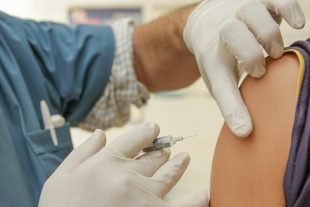
The vaccine is optional, but it will help us return to normal.
The government is following the prioritisation plan recommended by an independent group of experts (Joint Committee on Vaccination and Immunisation), which prioritises those at highest risk of catching the disease and suffering serious complications or dying from Covid-19.
Some of these vulnerable individuals will need support to make decisions about their health and welfare or may not have capacity to consent to the vaccine.
NHS England have produced guidance that says a person needs to give consent to receive the vaccine if they are able to make decisions for themselves.
This blog is for those who either are administering the vaccination or those who have the decision-making authority on behalf of someone who lacks capacity to consent themselves.
Those being vaccinated should be able to understand, retain, or communicate:
- the possible benefits in the simplest of terms
- the likely side effects and any individual risks should be understood
- what could happen if they don’t consent.
NHS England’s guidance states that patients should be provided with written information about the vaccination, but written consent is not required.
Why should you seek consent?
Based on both the current legal position and the standards expected of healthcare professionals, the person receiving a vaccine must agree before they are given the vaccine.
It’s important to assume a person has the ability to make their own decision unless proven otherwise. However, a lack of mental capacity to consent should not stop a vaccine being offered. There are additional steps that the vaccinator will need to take if the person lacks capacity to consent to the vaccine.
Understanding that not everyone is able to give consent
Where it’s been established that a person doesn’t have the mental capacity to consent to the Covid-19 vaccine, someone else can make a best interests decision for them, and it is necessary to understand who should make that decision.
Office of the Public Guardian (OPG) guidance for those administering vaccines
Healthcare professionals, allied health professionals or volunteers offering the vaccine to someone who may lack mental capacity to consent should first clarify if there is:
- a relevant Court of Protection Order (generally this is a deputyship order, but it might be an order of the court about this specific issue) or
- a Lasting Power of Attorney (LPA) for Health and Welfare in place.
The OPG offers a service where you can find out if someone has a lasting power of attorney (LPA) or a court-appointed deputy acting on their behalf. If there is an appointed deputy or attorney assigned to the individual, then they are likely to be the decision maker about whether the vaccine should be administered. The healthcare professional or individual administering the vaccine should first consult them.
If you need to find out if the patient has a registered attorney or appointed deputy, please refer to our OPG COVID pages for NHS and social care staff.
If the attorney or deputy does not consent to the vaccine being administered, the healthcare professional may consider that decision isn’t in the best interest of the individual. If so, the healthcare professional should seek legal advice from the relevant local authority or NHS body.
Where it has been established that the individual lacks capacity to consent and there is no attorney or deputy with appropriate authority, a best interests decision should be taken by the person administering the vaccine. This should be in line with the section 4 of the MCA. Consent can only come from the individual, or a health and welfare attorney or deputy. The vaccinator should not seek consent from a family member on the basis that they are ‘the next of kin’, or the holder of a property and financial affairs LPA/deputyship, to administer the vaccine.
Please refer to our OPG guidance for more information and guidance on best interests decisions and common health and welfare decisions.
Office of the Public Guardian (OPG) guidance for attorneys and deputies
When making a decision on behalf of someone who lacks capacity to decide if they should receive a Covid-19 vaccine, you should think about what their wishes would be if they were able to make this decision for themselves. Here’s a few things you can do in advance to ensure you are contacted for your decision:
- If the person lives in a care facility, tell the facility they must contact you for a decision in advance
- If the person lives alone, contact the local vaccination team to ensure you are contacted for a decision before the vaccine is given
The healthcare professional can only administer the vaccine if you have given your consent.
As an attorney or deputy, you do not need to attend the vaccine appointment. As long as you have given your consent on behalf of the person, someone else can take them to the vaccine appointment with your permission.
There is a required field to record the deputy or attorney’s consent or a best interests decision to vaccinate, or not. If the person giving consent is either an attorney or deputy, the name of that person and their relationship to the individual should also be recorded. This records only the decision and the discussions that have taken place with the donor or the person giving consent on someone’s behalf.
More information on making a best interests decision, for attorneys and deputies, is available, please refer to our OPG guidance.
Please refer to our OPG COVID pages for further details about being an attorney or deputy during this time
Need more information or do you have any questions?
Please refer to chapters 4 and 5 of the Mental Capacity Act Code of Practice for more information and guidance about how the MCA works in practice.
If you have any questions about this article, please contact us in the comments box below or email the OPG Communications Team.
2 comments
Comment by M Herdman posted on
This information was needed 8 weeks ago!
Now most Care home residents have been vaccinated, this is the group who are most likely to have LPA's in place.
Please be ahead of the game, or don't comment.
Comment by Jacquie CHENEY posted on
Excellent, clarity acheived by simplicity! Well done OPG